Agenesis of maxillary lateral incisors: To treat or not to treat?
- Dr Mo Almuzian

- Dec 29, 2020
- 3 min read
Tooth eruption
The maxillary lateral incisor erupts by the age of 7-9 years. Suppose the tooth fails to erupt after this age or six months of the contralateral incisor eruption or one year from the mandibular incisors' eruption, in that case, radiographic examination to confirm the developmental absence (tooth agenesis) becomes essential (Seehra et al., 2018).
Aetiologies and prevalence
Agenesis of the maxillary lateral incisors can be genetic, environmental or epigenetic factors (Khalaf et al., 2014). Its prevalence is 1-3% (Zilberman et al., 1990; Pinho et al., 2005; Arandi and Mustafa, 2018; Fujita et al., 2009) and it constitutes 24% of overall teeth agenesis (Khalaf et al., 2014). Bilateral agenesis of the maxillary lateral incisor is more common than unilateral agenesis. Females are more commonly affected than males with a ratio of 2:1 (Robertsson and Mohlin, 2000; Stamatiou and Symons, 1991).
Quality of life (QOL)
QOL may be defined as a person's sense of well-being that stems from satisfaction or dissatisfaction with the areas of life that are important to him/her' (Becker et al., 1993). QOL is a rapidly expanding area with over 1000 new articles indexed each year under the heading ‘quality of life' (Muldoon et al., 1998). Instruments to measure the QOL include (Guyatt et al. 1993):
• Direct interview;
• Telephone interview;
• Surrogate responders; and
• Self-completion questionnaires.
Oral-health-related quality of life (OHRQoL) has been defined as either a standard of health of oral and related tissues which enables an individual to eat, speak and socialize without active disease, discomfort, or embarrassment’. Examples for OHRQoL are Oral Health Impact Profile (OHIP) and Rosenberg’s Self-Esteem Scale. OHIP is an example of commonly used self-completion questionnaires developed by Slade in 1997 and consists of 14 questions. Higher OHIP score means the high negative impact of the treatment/ disease on the patient.
Problems
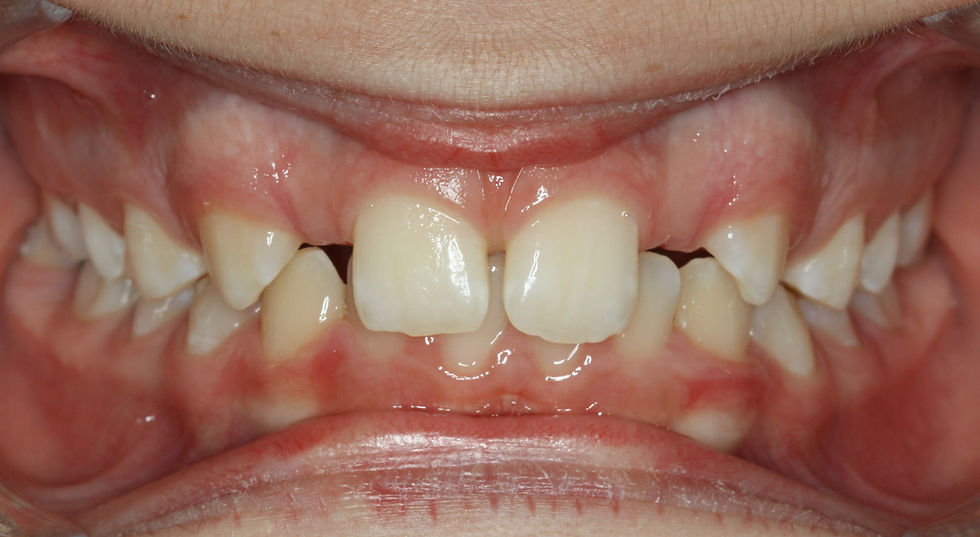
A congenitally missing lateral incisor is associated with an impact on self-perceived OHRQoL and self-esteem of the patients; these include unsightly space in the aesthetic zone, midline shift, reduced overjet, tipping of central incisors, rotations and a median diastema between the central incisors (Savarrio and McIntyre, 2005).
Management
Available treatment options for missing lateral incisors are:
• Orthodontic space closure (cuspid substitution),
• Space opening followed by prosthetic replacement using a bridge or implant-supported prosthesis,
• Space relocation (opening space between the premolars for an implant while accepting the canine in the lateral incisor position), and
• Auto-transplantation.
Treatment option depends on several factors (Savarrio and McIntyre, 2005; Kavadia et al., 2011; Ciğer and Telli, 1990; McNeill and Joondeph, 1973; Kokich and Kinzer, 2005).
Uncertainty
What is the impact of closing the space of missing lateral incisors on OHRQoL and self-esteem of the patients?
Update
European Journal of Orthodontics in their December 2020 issue published a single-blinded randomized controlled trial to answer these uncertainties.
The paper titled “Impact of oral-health-related quality of life and self-esteem on patients with missing maxillary lateral incisor after orthodontic space closure”.
A team from Brazil led by Dr Pithon undertook this trial which included 44 patients (17–49 years). Half of the cohort received orthodontic treatment to close the space, and the rest had no treatment (no sure how easy it is to get ethical approval). OHIP and Rosenberg’s Self-Esteem Scale were used to measure the impact of the intervention on the OHRQoL and self-esteem, respectively.
In summary, treatment resulted in significant improvement in the self-esteem and increasing the OHIP (P < 0.001); hence, leaving the case untreated means a negative impact on the OHRQoL and self-esteem of the patients. However, there was some limitation in the study, in particular, the timing of collecting the data from the patients, which might lead to some random and systematic errors.
What do you think?
PS: Credit to Dr Dalia Elbokle and Dr Haris Khan for sharing the review information of this post.




Comments